3 Ways to Report a Doctor

After dealing with chronic pain due to spine issues, Dr. L, my pain medicine doctor, wanted me to see Dr. S, a surgeon, to see if I needed surgery. Dr. L had been the bright light in my life after I took a fall from my horse and broke 4 vertebrae. He listened, validated my symptoms and concerns, and wanted to know what I felt I needed.
Dr. S was your typical surgeon with little to no interpersonal skills, rushing in, and jumping into his side of the conversation before I was able to get a word in. He looked at my imaging for two minutes, told me there was nothing he could do for me. So far, so good....
He then went into a tirade about how pain meds were evil, that I needed to stop them immediately, and just get on with my life. Go ride your horse and stop worrying about your pain.
With tears streaming down my face, I left the office feeling not only hopeless but ashamed that I needed pain meds.
I wanted to report him and tell everybody how terrible he was.
But, other than be...
Why We Need to Stop Demonizing All Doctors

Listen - I know dealing with doctors for rare diseases can be awful.
Medical trauma is real...I haven’t met a single rare disease patient who hasn’t
experienced it.
Sadly, we have to kiss a lot of frogs to find our prince (so to speak).
But, when we demonize doctors, we are the ones who are most hurt by it.
3 Reasons to Stop Demonizing Doctors
1. It makes you into the victim
YOU have the power and the right to choose your medical care and who you work with. It’s your body, your health, and your life!
You can’t change how each doctor treats you but you can change how you respond to it so you are no longer a victim.
Don’t let one person, who you don’t agree with, have the power to upset you and deny you the care you need.
Protect yourself by saying “Not the right doctor...next?”
2. It prevents us from holding them accountable
Doctors say a lot of crappy things to rare disease patients. Sometimes, their behavior goes beyond not being the right doctor to abuse, mistreatment, ...
Why It’s Important to Disagree With Your Doctor

Raise your hand if you have ever disagreed with a doctor?
Maybe I should ask how many doctors have you not disagreed with?
How many doctors are happy when you disagree with them?
It can be hard, especially for those us who don’t like conflict, to speak up and disagree with our doctors but let’s talk about why it is so important.
You are the Controlling Partner
Ideally, our relationship with our doctor is a partnership where we work together toward the same goal but even partners disagree. Disagreements may occur on the goal, testing, diagnosis, or which treatment to be used.
The best partnerships build off the strengths of each of the partners. In this case, you are the expert on your body - what you experience, how it reacts, and your goals. Your doctor is an expert on medicine (in general) - their understanding of the disease, diagnosis, and treatment.
So, as the controlling partner in this partnership, it is critical that you speak up when there are things that you ...
Medical Trauma - Is it Real?
Do you deal with the effects of medical trauma?
Have you been told you need to get over it and suck it up?
Is medical trauma real?
It started out gradually, one day I noticed my arm was aching and it hurt to write or to be on the computer. Pretty soon, I had a stabbing, unrelenting pain that spread to my neck and shoulder blade - it left me in tears and unable to sleep well. Before long my forearm was screaming in pain and my hand was numb and tingling.
I approached it in the ‘tried and true’ method of just ignore it and it will go away. No luck. I tried resting it but that didn't help either. Soon the pain was so bad I couldn’t use my arm and even walking was uncomfortable.
“Please don’t let this be another cervical disc and stenosis problem or Parsonage-Turner Syndrome, a rare neurologic disease,” I muttered to myself. My cervical fusion in Aug 2019 had gone well but it was a tough recovery and I really didn’t want to repeat that. For several years prior to that, I had dealt with...
How Does Your PCP Measure Up?
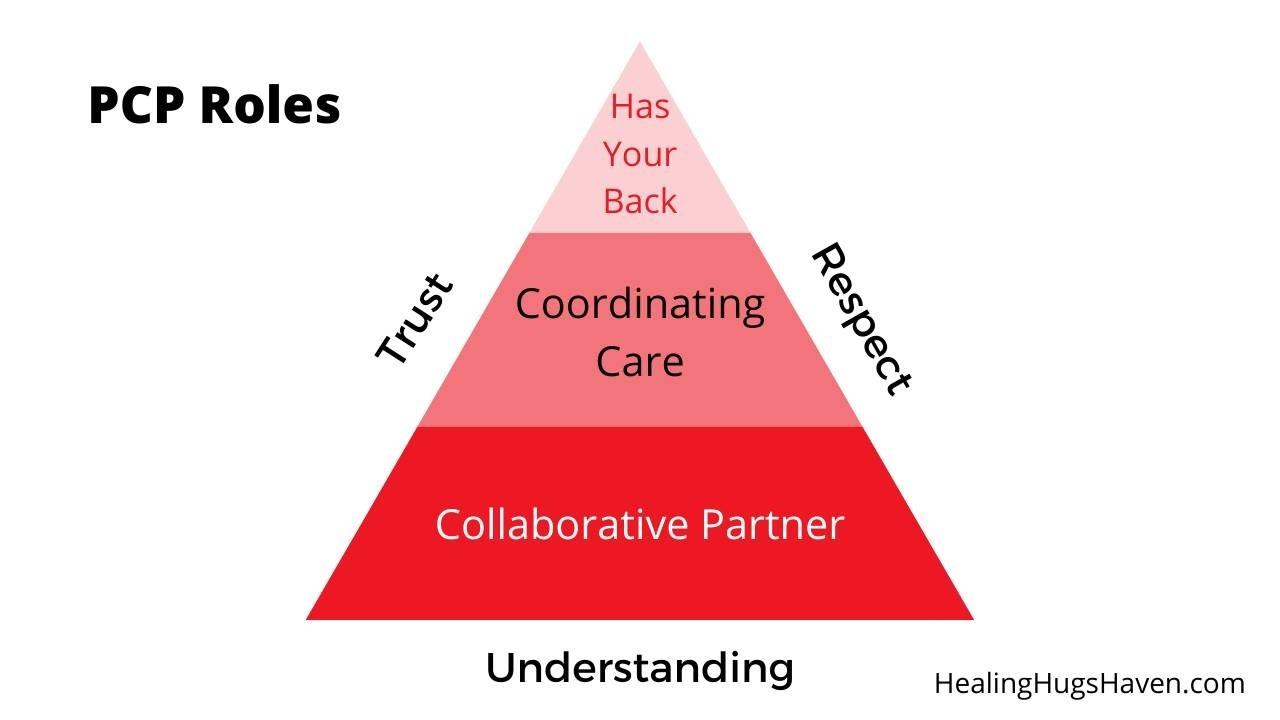
Your PCP refers you to a specialist, let's say they are a headache specialist named Dr. H (for headache), to get help with your migraines that are common with your rare disease. Dr. H has no experience with your rare disease but is a headache specialist.
After seeing Dr. H, your PCP shares with you Dr. H decided that you don’t really have migraines and that you are a drug seeker.
Now what?
We all know that our PCP’s are helpful when we have strep throat or need a referral to a specialist. But to be fully supported there are additional roles that are critical for your PCP to be engaged and willing to perform.
1. Collaborative Partner
“Collaborative Partner - two or more parties engaged and working together on the same activity”
How many times have you brought up an issue only to have your PCP dismiss it and move on to their next item?
You are the main stakeholder in this relationship. It’s your health, your health care, and your life.
You are the expert on your ...
Can the Wrong Doctor Be Dangerous?

As in so many areas of life, it is hard or often impossible to know 'what you don't know' or to recognize what hidden issues or dangers are out there.
When you are dealing with doctors and medical issues, what you don't know and the hidden dangers of staying with the wrong doctor can be disastrous and even life-threatening.
The effects of staying with 'a wrong doctor' can vary from mild frustration to long term effects on the quality of your healthcare.
Changing doctors isn't easy or for the faint of heart
I get it. Finding, meeting and working with a new doctor is a lot of work and can be scary too.
Let's take a closer look at some of the hidden dangers of staying with the wrong doctor.
Danger #1: Emotional or psychological effects
When a doctor is dismissive or assumes the issues are from anxiety or depression, it can have a huge impact on you and your loved one's emotional and mental health.
How many of us have been told that it is anxiety? Or if you make them go to schoo...
Home Monitoring or ER? Updated Anaphylaxis Recommendations
Have you heard about the new anaphylaxis management algorithm?
If you or someone you love has had anaphylaxis that required an epi-pen, it is likely that you were told to call 911 and immediately go to the ER for observation.
Last week, FARE updated their recommendations to include COVID-19 into the risk/benefit balance of monitoring at home vs. an ER visit. This is especially important in areas where ERs are swamped with COVID-19 patients although most ERs have new procedures to screen for COVID-19 when getting checked in along with a focus on minimized time spent with any patient to lessen risk of transmission.
As you can imagine, these new recommendations have caused a bit of controversy and concern in the food allergy and mast cell disease world.
Let’s take a closer look at the new recommendations and why they are being made.
Dr. Thomas B. Casale, the chief medical advisor for operations with FARE (Food Allery Research & Education) and professor of medicine and p...
Top 10 Reasons Rare Disease Patients are Pandemic Pros

Rare Disease Patients are...
-
Pros at limiting infection and cross-contamination, sporting facemasks, washing hands, and effective cleaning
-
Experienced at social isolation including homeschooling, and other creative options, work from home solutions and, finding support online
-
Used to handling emergencies, monitoring symptoms at home, and employ multiple rehydration techniques
-
Familiar with doing research by reading research articles, crowdsourcing ideas, and resources
-
Practiced at treasure hunting food, supplies, meds and necessities (TP anyone?)
-
Stocked with medical equipment and supplies to rival a medical supply company (BP cuff, pulse ox, electrolytes, etc)
-
Blessed with Mad MacGyver skills to adapt and figure things out.
-
Experts at knowing our own bodies, symptoms, medical history, meds, and what we need
- Ph.D.s in dealing with red-tape and bureaucracy
-
Resilient, used to living with uncertainty, the unknown and finding meaning in...
Uncharted Territory - Doctor's Appointments in the time of COVID-19

Getting rare disease care has never been easy but with the coronavirus outbreak, it has become even harder. Clinics are closing, surgeries are being rescheduled and long-awaited appointments are being postponed.
Many of you may have had things canceled or postponed. As disappointing as this is, it is important to realize that this is being done to help our medical system handle the coronavirus outbreak from a logistic point while also trying to optimize your safety as well.
Your doctor, their clinic and/or hospital will be following recommendations by the CDC (Center for Disease Control) and ACS (American College of Surgeons) along with careful consideration of your specific medical case to decide what can and should be rescheduled.
Our doctors were struggling to survive in a broken medical system before but now they are entering the totally unchartered territory of providing medical care during a pandemic. The medical system is being stressed beyond anything that it ha...
3 Ways for Rare Disease Patients to Prepare for Coronavirus
Depending on where you live, how much you follow the news and your general personality type, you may or may not be concerned about COVID-19. Panicking doesn't help anyone but being prepared may help and certainly won't hurt.
There are a lot of general recommendations out there but here are several specific ways that you can prepare as a rare disease patient.
1. Get extra prescription and OTC meds to have on hand.
- There is the potential for drug shortages based on the amount of medication we import that gets produced in India with ingredients coming from China. As reported in The Wall Street Journal If Coronavirus-Stricken China Can’t Export Medicine, the World Is in Trouble, "China is the source of a large percentage of basic drug ingredients." Most drug manufacturers keep a 2-3 month supply on hand so hopefully, the Chinese factories will be back online before it becomes a big issue. But, given that rare disease patients take quite a few medications and that they often need...


